Transradial Carotid Artery Stenting
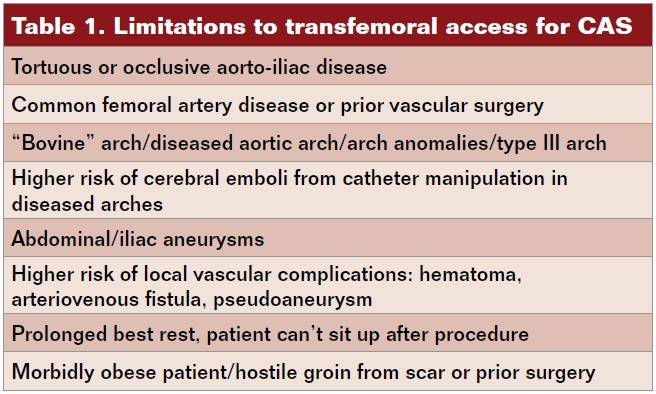
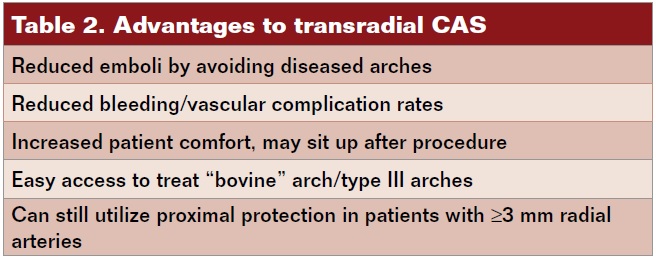
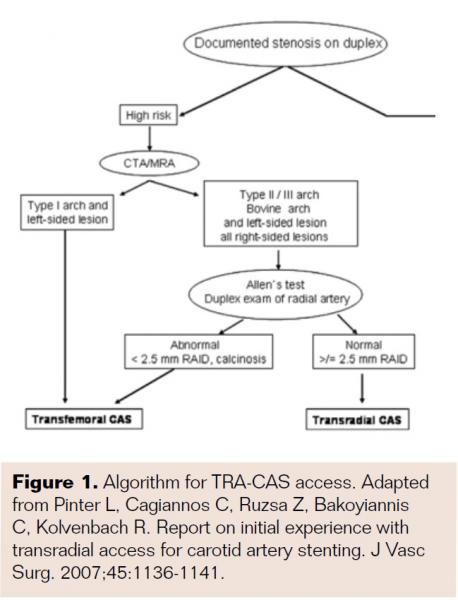
Carotid artery stenting (CAS) is now a well-established technique for the treatment of both symptomatic and asymptomatic cervical bifurcation disease. CAS procedures are typically performed from a femoral access, but there are limitations to this route (Table 1). Multiple single-center studies and randomized trials have proven the safety, efficacy, and reduced vascular complication rates of transradial (TR) catheterization and percutaneous coronary intervention (PCI).1 These same techniques have been adapted for the performance of CAS. Transradial CAS has several potential advantages compared with transfemoral (TF) access (Table 2). Limitations of TRA-CAS will also be reviewed (Table 3). Herein, we present a case report of TRA-CAS, review the data, and offer a suggested CAS access algorithm (Figure 1).

Case Report
The patient is a morbidly obese 70-year-old male with past medical history of severe tobacco abuse with oxygen-dependent chronic obstructive pulmonary disease (COPD), coronary artery disease (CAD) with myocardial infarction in 1997 with subsequent coronary artery bypass graft x4, prior history of alcohol abuse having quit in 1979, insulin-dependent diabetes mellitus, hypertension, hyperlipidemia, obstructive sleep apnea (OSA), and hypothyroidism with known right internal carotid artery stenosis, confirmed by recent computed tomography angiography (CTA) to now have >80% stenosis. He was felt to be high risk for carotid endarterectomy as well as for transfemoral CAS due to OSA, short thick neck, oxygen-dependent COPD, CAD, and morbid obesity. For these reasons, he was referred for transradial CAS.
Technique
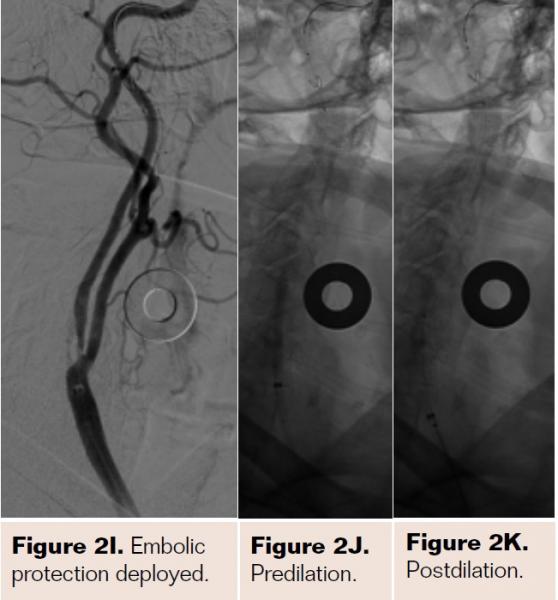
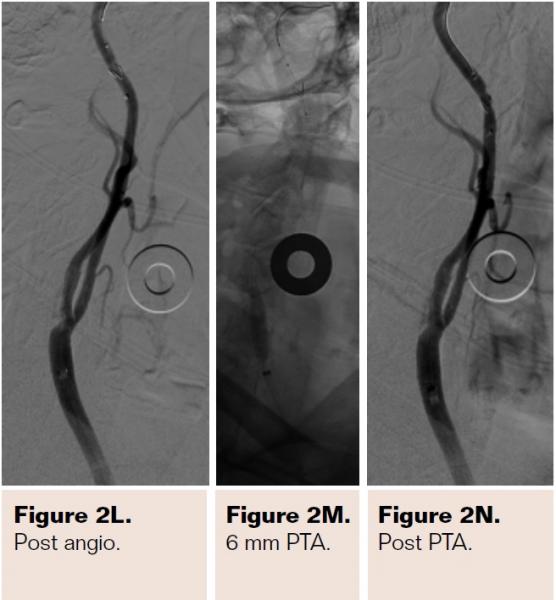
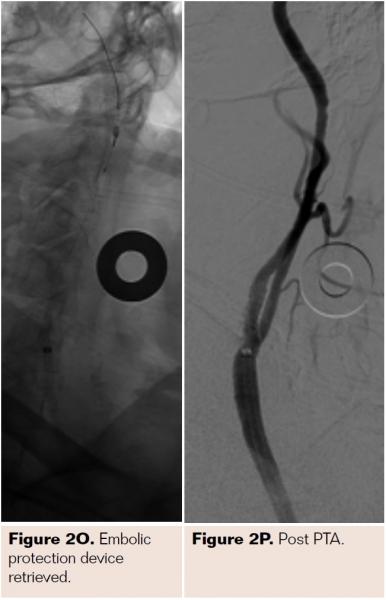
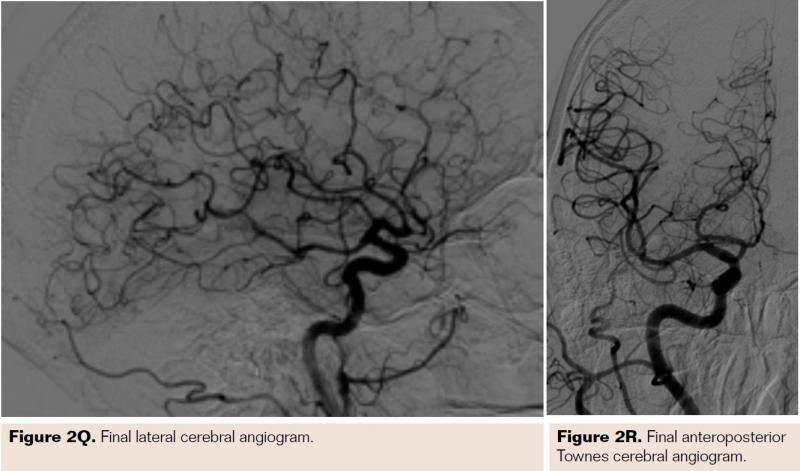
Pretreatment with dual-antiplatelet therapy (DAPT) was started 4 days prior to the procedure with aspirin and clopidogrel, with 600 mg loading dose of clopidogrel and 80 mg dose of atorvastatin the morning of the procedure. The right radial artery was accessed with a 6 Fr Terumo radial sheath, but intraarterial nitroglycerin was not administered due to a prior history of profound hypotension with sublingual nitroglycerin. Verapamil was withheld due to a systolic blood pressure of 130 mm Hg. Both right and left anterior oblique arch aortograms with a 5 Fr straight pigtail catheter demonstrated patency of the proximal great vessels, a type I aortic arch, and a calcified proximal right internal carotid artery (ICA) high-grade stenosis with patent right external carotid artery (ECA). The right common carotid artery (CCA) was selected with 5 Fr internal mammary (IM) diagnostic catheter that confirmed an 85% proximal right ICA stenosis. A soft-angled .035˝ Glidewire (Terumo) was advanced into the right ECA, exchanged out for an Amplatz .035˝ super-stiff wire (Boston Scientific), followed by removal of the diagnostic catheter, and radial sheath. A 6 Fr Shuttle sheath (Cook Medical) was delivered into the distal right CCA. After intracranial angiography, a NAV-6 Emboshield (Abbott Vascular) was deployed in the distal extracranial ICA, followed by predilation with a 4 x 30 mm Trek (Abbott Vascular), and deployment of a 7 x 30 mm Precise self-expanding stent (Cordis). Postdilation was performed with a 5 x 20 mm Maverick NC balloon (Boston Scientific), and then with a 6 x 20 mm Aviator balloon (Cordis) in order to then deliver the retrieval catheter. After repeat angiography confirmed an excellent result, the Shuttle was removed, and hemostasis achieved with TR band (Terumo) (Figures 2A-2R).
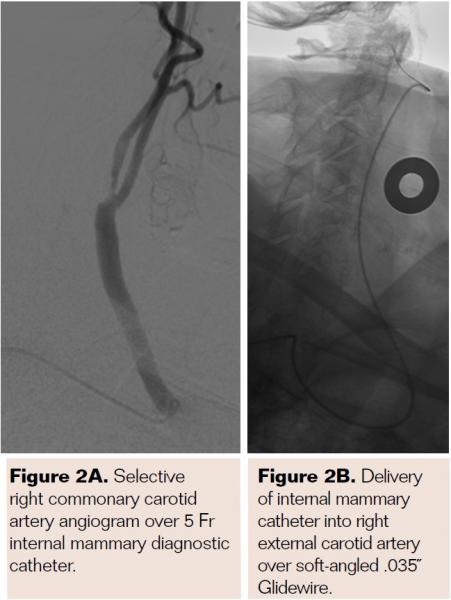
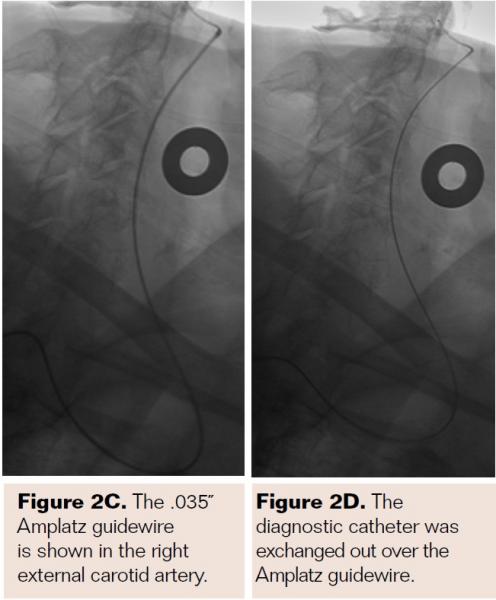
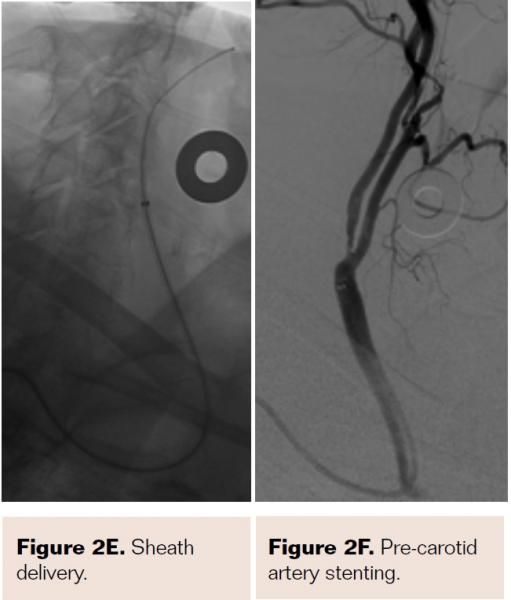
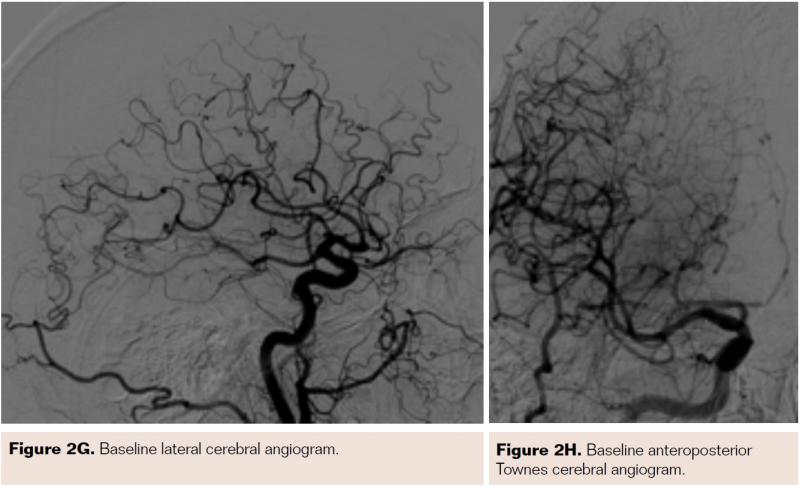
PreProcedure Planning for Transradial CAS
All patients should have CTA or magnetic resonance angiography (MRA) imaging to plan CAS access (Figure 1). Several authors have noted a lower procedural success rate in cannulation of the left CCA in patients with type I aortic arches from the right radial artery.3-7 Folmar et al noted successful CAS outcomes in 97% of right CAs, 80% of bovine CAs, and only 54% of left CAs.3 Preprocedure imaging identifies atherosclerotic and calcific disease, arch anomalies, and unfavorable anatomy (acute angles of <50°) that predict technical difficulties, thus allowing for reduced stroke risk and need for crossover access. Typically, DAPT is started at least 4 days before the procedure with a loading dose of clopidogrel or ticagrelor prior to the procedure.
Radial Access Technique
Ideally, the radial artery should be imaged with duplex ultrasound to determine the size of the vessel, particularly if an 8 Fr sheath for proximal protection is planned. A negative Allen’s test is performed, the wrist hyperextended, local anesthesia is administered, and the artery punctured with a micropuncture needle. A 5 Fr or 6 Fr radial sheath is inserted, followed by a spasmolytic cocktail, eg, 200 µg nitroglycerin and 2.5 mg of verapamil, and systemic anticoagulation with heparin, or preferably, bivalirudin, is given aiming for a target activated clotting time of >250 seconds.
Most reported series have used the right radial artery due to ease of cannulation of the right CCA and bovine left CCA, avoidance of catheter manipulation in the arch, and for the familiarity and ease of use for most interventionists. Patel et al performed CAS from the contralateral RA in 20 patients after preoperative Doppler confirmed adequate radial size, absence of tortuosity, or atherosclerosis.4 They noted 4 of 8 left CAS procedures failed due to technical reasons, but were able to be successfully performed via femoral approach. Nevertheless, they advocate for left RA access for right ICA-CAS if there is a severe angle between the right subclavian artery and right CCA. In cases of radial access failure, the ulnar may be used. The ulnar artery is straighter, larger, and less prone to spasm, but is deeper and next to the ulnar nerve. Retrograde ulnar and radial artery angiography is recommended to aid in optimal procedure planning and to avoid unfavorable anatomy.8-10
Transbrachial CAS
The transbrachial (TB) approach is not routinely recommended due to the greater difficulty with vessel access (particularly without ultrasound guidance) and the greater frequency and severity of complications. These may include hand ischemia, distal embolization, brachial sheath hematoma, median nerve injury, and compartment syndrome.11 The multicenter, randomized Access study, which compared TR, TB, and TF complications, found TB access to have the highest rate of major complications (2.3% TB vs 2.0% TF vs 0% TR).12 Nevertheless, the TB approach is often chosen if the radial pulse is weak, if the patient had prior radial artery catheterization, if proximal embolic protection is planned, and in women with small radial arteries.
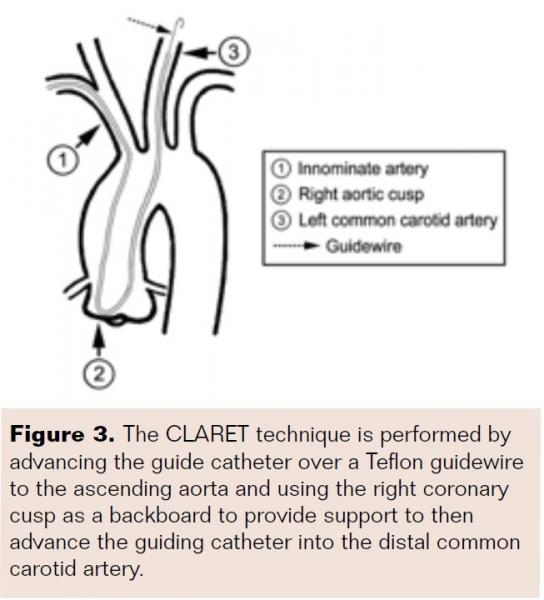 Several investigators have reported the feasibility of TB-CAS.13-16 Fang et al first reported on the CLARET (catheter looping and retrograde engagement technique) for CAS using TR access for patients <175 cm and TB access for those >175 cm in 61 patients (Figure 3).17 Two patients developed pseudoaneurysm with arteriovenous fistula requiring surgical repair. Montorsi et al performed TR-CAS/TB-CAS for bovine left ICA disease in 32 and 28 patients, respectively. Two of the 28 TB patients (3.3%) developed complications – 1 thrombosis and 1 pseudoaneurysm, both treated surgically.6 Their larger follow-up series included 154 TR and 60 TB patients. Three TB patients (1.96%) developed vascular complications – 1 brachial artery pseudoaneurysm and 2 brachial artery thromboses, all treated surgically.19
Several investigators have reported the feasibility of TB-CAS.13-16 Fang et al first reported on the CLARET (catheter looping and retrograde engagement technique) for CAS using TR access for patients <175 cm and TB access for those >175 cm in 61 patients (Figure 3).17 Two patients developed pseudoaneurysm with arteriovenous fistula requiring surgical repair. Montorsi et al performed TR-CAS/TB-CAS for bovine left ICA disease in 32 and 28 patients, respectively. Two of the 28 TB patients (3.3%) developed complications – 1 thrombosis and 1 pseudoaneurysm, both treated surgically.6 Their larger follow-up series included 154 TR and 60 TB patients. Three TB patients (1.96%) developed vascular complications – 1 brachial artery pseudoaneurysm and 2 brachial artery thromboses, all treated surgically.19
Carotid Angiography & Intervention
Various 5 Fr diagnostic catheters may be used for performing selective carotid angiography, including Simmons 1 and 2, IM, Berenstein, JR 4, and JB1 shapes. The AR 2 may also be used for selecting a bovine left CCA. The group from Taiwan utilizes a 6 Fr Kimny guiding catheter (GC) for diagnostic angiography, and the 7 Fr Kimny GC for the intervention, utilizing the CLARET technique, where the catheters are advanced against the right aortic cusp for support.
Following angiography, an exchange-length extra-support wire (Supracore, Amplatz super-stiff, TAD II or stiff Glidewire) is advanced into the ECA, followed by removal of the diagnostic catheter and radial sheath. A 6 Fr sheath is then advanced into the distal CCA for distal embolic protection cases, or an 8 Fr sheath for MoMa proximal embolic protection (Medtronic). If a 7 Fr GC (eg, Kimny or XF 40 [Boston Scientific]) was chosen (compatible with 5 Fr stents and distal filters), it is then similarly advanced into the distal CCA. This is the anchoring technique, which is used for straightforward anatomy. Stenting of the carotid artery is then performed in the usual fashion, followed by hemostasis of the access site with a TR band.
Due to the acute angles between the subclavian artery and right CCA and the innominate and left CCA, it may be difficult to advance the GC or sheath into the distal CCA, chiefly due to insufficient support. Various techniques may be used to overcome these obstacles. The first is the telescopic technique, in which the GC or sheath is delivered over a 125 cm braided 5 Fr diagnostic catheter (Simmons 1 or 2), similar to TF-CAS. The diagnostic catheter is delivered into the distal CCA, followed by advancement of the GC or sheath.
The CLARET (catheter looping and retrograde engagement technique) may also be used, and is performed by advancing the GC over a Teflon guidewire to the ascending aorta and using the right coronary cusp as a backboard to provide support to then advance the GC into the distal CCA.
Proximal embolic protection CAS is increasingly popular as more studies report reduction in periprocedural stroke rates.19-32 Trani et al33 first reported 3 cases of TR-CAS using the 8 Fr MoMa device and Montorsi et al18 performed 61 cases using the MoMa device from either a TR30 or TB31 access. The TB access was preferred for CCA diameters >8 mm to allow for delivery of up to a 10 mm Cristallo stent (Medtronic) or if the radial pulse was weak or had prior radial artery catheterization. Most of these patients (52%) had bovine configuration. Only 1 patient (1.6%) could not have the MoMa device positioned and was crossed over to TF approach, and another was transitioned to a distal embolic protection (DEP) device because the MoMa device was too short to engage the ECA from a radial access. In 16 cases, the first attempt to deliver the MoMa was unsuccessful using standard techniques, but was able to be delivered by removing the mandrel wire and adding a second wire in the main channel (the “NoMa2” technique). Only 1 major vascular complication occurred (brachial artery pseudoaneurysm) and was successfully repaired surgically. At an average follow-up of 8.1 ± 7.5 months, radial artery occlusion (RAO) occurred in 2 of 30 patients (6.6%).
Discussion
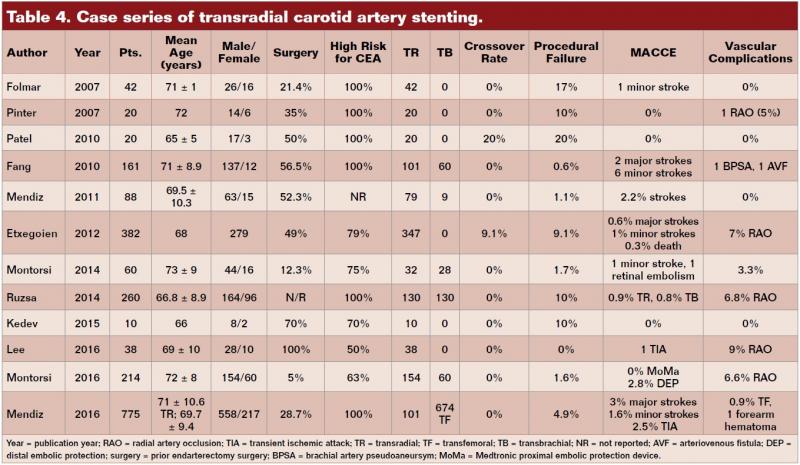
Several case reports have confirmed the utility of radial access for CAS.13,34-41 The larger series are summarized in Table 4. Folmar confirmed the feasibility of TR-CAS in 42 high surgical risk patients, of whom 9 were symptomatic. Bivalirudin was used as the anticoagulant, 74% of cases were done with a 6 Fr Shuttle, the remainder with a 5 Fr sheath. Overall success was achieved in 35/42 patients (83%) including 28/29 (97%) right, 4/5 (80%) bovine, but only 7/13 (54%) left carotid stenoses.3 Failures were due to inadequate support to deliver the sheath to the left CCA. Only 1 patient sustained a stroke, and there were no vascular complications. A follow-up two-center retrospective study of 383 patients documented overall success in 347/383 (91%), with 93% right, 88% bovine, and 88% left CA. All TR failures due to inadequate support were successfully performed from the TF approach. There were 2 major strokes (0.6%), 3 minor strokes (1%), 10 transient ischemic attacks (3%), no myocardial infarctions, and 6% of patients had asymptomatic RA occlusion.5
Fang et al reported on their experience using CLARET to perform TR-CAS and TB-CAS on 161 patients. TB access was used for patients taller than 175 cm. CAS was performed using a 7 Fr Kimny GC with only 1 failure, which was due to ECA occlusion.17 Two patients experienced major stroke, 6 had minor stroke, and two TB patients developed pseudoaneurysm requiring surgical repair. They then compared sheathless TRA-CAS with the previously published TB-CAS using 7 Fr Kimny GC in 38 patients, with a 100% success rate. One patient experienced a transient ischemic attack and 3 patients (9%) developed RAO at 1 year.16
Pinter performed TR-CAS on 20 consecutive patients (7 symptomatic) with no deaths, strokes, or myocardial infarctions.2 Two patients could not be completed via RA access due to intense spasm in 1 case, and inability to cannulate the left CCA in the other. Both were done from the TF approach. Patel demonstrated the feasibility of contralateral TRA for CAS in 20 patients (40% symptomatic) who all had preoperative Doppler evaluation of RA size to rule out loops, kinks, tortuosity, or atherosclerosis. Only 4 out of 8 patients with left CCA were able to be cannulated via TR access, but the rest were able to be completed via TF access. One patient had a transient ischemic attack, with no vascular complications or bleeding.4
Mendiz et al initially reported on 88 patients (46 symptomatic) with 98.8% TR access and 96.6% procedural success.42 Two patients had procedural stroke (one ischemic, the other hemorrhagic), with no myocardial infarctions or deaths, and no vascular complications. Their 16-year experience was recently reported on 775 consecutive high surgical risk patients treated with TR-CAS (n = 101) and TF-CAS (n = 674).43 Procedural success was 100%, with a 4.9% TR crossover rate, and 2% stroke rate in TR patients and 2.7% in TF patients. All crossovers were due to difficult carotid cannulation or insufficient support in type III arches. One TR patient had a forearm hematoma treated medically, with a 0.9% TF vascular complication rate.
Montorsi et al demonstrated the utility of TR (n = 32) and TB (n = 28) treatment of 60 consecutive patients with left ICA stenosis and bovine arch. Proximal protection was used in 15 cases.6 Incidence of in-hospital major adverse cardiovascular and cerebral event (MACCE) was 2% in the TR group and 3.6% in the TF group. Two patients with TB access had vascular complications treated surgically. Montorsi et al subsequently reported on 31 TB patients and 30 TR patients treated with proximal embolic protection, and 153 with DEP.18 Fifty-two percent of the MoMa-treated patients had bovine left ICA, with only 1 case where the MoMa device could not be delivered. In 16 cases, the MoMa device was not able to be delivered on first attempt, but was able to be delivered using a no-mandrel 2-wire technique (the “NoMa-2” technique). There was a 7.1% crossover rate in the DEP group due to technical difficulty engaging the target vessel. MACCE rate was 0% in the MoMa group and 2.8% in the DEP group (P=.18). One MoMa-treated patient developed a brachial pseudoaneurysm treated with surgery, and two DEP patients required brachial surgical repair. At 8.1-month follow-up, 6.6% of MoMa radial and 3.2% of DEP radial arteries were occluded. Fluoroscopy times (15.8 min vs 12.75 min) and contrast amounts (135 mL vs 107 mL) were higher with DEP, but overall radiation exposure was similar.
The RADCAR study was a randomized comparison of TR and TF approach for CAS in 260 patients.7 Type III arches were more common in the TR group. Crossover rate was 10% in the TR group and 1.5% in the TF group. All cannulation failures due to severe angulation of the CCA origins were successfully treated from the crossover access. Procedure and fluoroscopy times were not significantly different, but the radiation dose was higher in the TR group. There were no differences in MACCE rates. Major and minor vascular complications were 2.3% major/4.6% minor in the TF group vs 1.5% major/7.8% minor in the TR group. Asymptomatic RAO occurred in 6.8% of the TR group. New, lower-profile 5 Fr stents and micromesh stents will likely expand the number of patients eligible for TR-CAS.10,44,45
Conclusion
TRA-CAS is safe and efficacious, with high success rates and very low vascular complication rates. Experienced TR operators are able to achieve low MACCE rates that are comparable with TF access. Consider TRA-CAS for patients with peripheral arterial disease, morbid obesity, and complex aortic arch anatomy. Although proximal embolic protection is possible with TR access, it is limited by vessel size, and for these patients, and those with left CA lesions with type I arch, TF access is still preferred.
Peter A. Soukas, MD, FACC, FSVM, FSCAI, FACP is the Director of Vascular Medicine & Interventional PV Lab, Director of the Brown Vascular & Endovascular Medicine Fellowship, The Miriam & Rhode Island Hospitals, and an Assistant Professor of Medicine, The Warren Alpert School of Medicine of Brown University, Cardiovascular Institute, 208 Collyer St. Suite 100, Providence, RI 02906. Email: psoukas@lifespan.org
References
- Ferrante G, Rao SV, Juni O, et al. Radial versus femoral access for coronary interventions across the entire spectrum of patients with coronary artery disease: a meta-analysis of randomized trials. JACC Cardiovasc Interv. 2016;9:14-19.
- Pinter L, Cagiannos C, Ruzsa Z, Bakoyiannis C, Kolvenbach R. Report on initial experience with transradial access for carotid artery stenting. J Vasc Surg. 2007;45:1136-1141.
- Folmar J, Sachar R, Mann T. Transradial approach for carotid artery stenting: a feasibility study. Catheter Cardiovasc Interv. 2007;69:355-361.
- Patel T, Shah S, Ranjan A, Malhotra H, Pancholy S, Coppola J. Contralateral transradial approach for carotid artery stenting: a feasibility study. Catheter Cardiovasc Interv. 2010;75:268-275.
- Etxegoien N, Rhyne D, Kedev S, Sachar R, Mann T. The transradial approach for carotid artery stenting. Catheter Cardiovasc Interv. 2012;80:1081-1087.
- Montorsi P, Galli S, Ravagnani PM, et al. Carotid artery stenting in patients with left ICA stenosis and bovine aortic arch: a single-center experience in 60 consecutive patients treated via the right radial or brachial approach. J Endovasc Ther. 2014;21:127.
- Ruzsa Z, Nemes B, Pintér L, et al. A randomised comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR (RADial access for CARotid artery stenting) study. EuroIntervention. 2014;10:381-391.
- Ruzsa Z, Sasko K. Transradial/transbrachial carotid artery stenting with proximal or distal protection: a promising technique for the reduction of vascular complications and stroke. J Endovasc Ther. 2016;23:561-565.
- Fang HY, Wang Y, Zheng JT, Wu CJ. Transulnar carotid artery stent placement. Catheter Cardiovasc Interv. 2013;81:709-712.
- Kedev S, Petkoska D, Zafirovska B, Vasilev I, Bertrand OF. Safety of slender 5Fr transradial approach for carotid artery stenting with a novel nitinol double-layer Micromesh stent. Am J Cardiol. 2015;116:977-981.
- Heenan SD, Grubnic S, Buckenham TM, Belli AM. Transbrachial arteriography: indications and complications. Clin Radiol. 1996;51:205-208.
- Kiemeneij F, Laarman GJ, Odekerken D, Slagboom T, can der Wiecken R. A randomized comparison of percutaneous transluminal coronary angioplasty by the radial, brachial and femoral approached: the Access study. J Am Coll Cardiol. 1997;29:1269-1275.
- Shaw JA, Gravereaux EC, Eisenhauer AC. Carotid stenting in the bovine arch. Catheter Cardiovasc Interv. 2003;60:566-569.
- Ventoruzzo G, Biondi-Zoccai G, Bellandi G. Commentary: choose the appropriate access route in bovine arch and you will turn a complex left carotid artery stenting procedure into a simple one. J Endovasc Ther. 2014;21:137-139.
- Montorsi P, Galli S, Ravagnani P, et al. Carotid stenting through the right brachial approach for left internal carotid artery stenosis and bovine aortic arch configuration. Eur Radiol. 2009;19:2009-2015. Epub 2009 Mar 11.
- Lee WC, Fang HY, Chen HC, et al. Comparison of a sheathless transradial access with looping technique and transbrachial access for carotid artery stenting. J Endovasc Ther. 2016;23:516-520.
- Fang HY, Chung SY, Sun CK, et al. Transradial and transbrachial arterial approach for simultaneous carotid angiographic examination and stenting using catheter looping and retrograde engagement technique. Ann Vasc Surg. 2010;24:670-679.
- Montorsi P, Galli S, Ravagnani PM, et al. Carotid artery stenting with proximal embolic protection via a transradial or transbrachial approach: pushing the boundaries of the technique while maintaining safety and efficacy. J Endovasc Ther. 2016;23:549-560.
- Ansel GM, Hopkins LN, Jaff MR, et al. Investigators for the ARMOUR pivotal trial. Safety and effectiveness of the INVATEC MoMa proximal cerebral protection device during carotid artery stenting: results from the ARMOUR pivotal trial. Catheter Cardiovasc Interv. 2010;76:1-8.
- Cano, MN, Kambara AM, Silvia JF, et al. Randomized comparison of distal and proximal cerebral protection during carotid artery stenting. JACC Cardiovasc Interv. 2013;6:1203-1209.
- Giri J, Parikh SA, Kennedy KF, et al. Proximal versus distal embolic protection for carotid artery stenting: a national cardiovascular data registry analysis. JACC Cardiovasc Interv. 2015;8:609-615.
- Stabile E, Biamino G, Sorropago G, Rubino P. Proximal endovascular occlusion for carotid artery stenting. J Cardiovasc Surg (Torino). 2013;54:41-45.
- de Castro-Afonso LH, Abud LG, Rolo JG, et al. Flow reversal versus lter protection: a pilot carotid artery stenting randomized trial. Circ Cardiovasc Interv. 2013;6:552-559.
- Montorsi P, Caputi L, Galli S, et al. Microembolization during carotid artery stenting in patients with high-risk, lipid-rich plaque. A randomized trial of proximal versus distal cerebral protection. J Am Coll Cardiol. 2011;58:1656-1663.
- Bijuklic K, Wandler A, Hazizi F, Schofer J. The PROFI study (Prevention of Cerebral Embolization by Proximal Balloon Occlusion Compared to Filter Protection During Carotid Artery Stenting): a prospective randomized trial. J Am Coll Cardiol. 2012;59:1383-1389.
- Stabile E, Salemme L, Sorropago G, et al. Proximal endovascular occlusion for carotid artery stenting: results from a prospective registry of 1,300 patients. J Am Coll Cardiol. 2010;55:1661-1667.
- Nikas D, Reith W, Schmidt A, et al. Prospective, multicenter European study of the GORE flow reversal system for providing neuroprotection during carotid artery stenting. Catheter Cardiovasc Interv. 2012;80:1060-1068.
- Clair DG, Hopkins LN, Mehta M, et al; the EMPiRE Clinical Study Investigators. Neuroprotection during carotid artery stenting using the GORE flow reversal system: 30-day outcomes in the EMPiRE clinical study. Catheter Cardiovasc Interv. 2011;77:420-429.
- Reimers B, Sievert H, Schuler GC, et al. Proximal endovascular flow blockage for cerebral protection during carotid artery stenting: results from a prospective multicenter registry. J Endovasc Ther. 2005;12:156-165.
- Coppi G, Moratto R, Silingardi P, et al. PRIAMUS: PRoximal flow blockage cerebral protectIon during cArotid stenting. Results from a MUlticenter Italian regiStry. J Cardiovasc Surg (Torino). 2005;46:219-227.
- Rabe K, Sugita J, Gödel H, Sievert H. Flow-reversal device for cerebral protection during carotid artery stenting – acute and long-term results. J Interv Cardiol. 2006;19:55-62.
- Ohki T, Parodi J, Veith FJ, et al. Efficacy of a proximal occlusion catheter with reversal of flow in the prevention of embolic events during carotid artery stenting: an experimental analysis. J Vasc Surg. 2001;33:504-509.
- Trani C, Burzotta F, Coroleu SF. Transradial carotid artery stenting with proximal embolic protection. Catheter Cardiovasc Interv. 2009;74:267-272.
- Castriota F, Cremonesi A, Manetti R, Lamarra M, Noera G. Carotid stenting using radial artery access. (Letter). J Endovasc Surg. 1999;6:385-386.
- Janjua N, Verma N, Alkawi A, Kirmani JF, Qureshi AI. Carotid stent-supported angioplasty via radiobrachial route. J Neuroimaging. 2006;16:212-215.
- Harjai KJ, Quenneville R, Safian RD, Schreiber T. Stenting of anomalous left carotid artery using a radial artery approach. Catheter Cardiovasc Interv. 2004;61:286-288.
- Yoo BS, Lee SH, Kim JY, et al. A case of transradial carotid stenting in a patient with total occlusion of distal abdominal aorta. Catheter Cardiovasc Interv. 2002;56:243-245.
- Gan HW, Bhasin A, Wu CJ. Transradial carotid stenting in a patient with bovine arch anatomy. Catheter Cardiovasc Interv. 2010;75:540-543.
- Maciejewski D, Pieniek P, Tekieli L, et al. Transradial approach for carotid artery stenting in a patient with severe peripheral arterial disease. Postepy Kardiol Interwencyjnej. 2014;10:47-49.
- Levy EI, Kim SH, Bendok BR, Qureshi AI, Guterman LR, Hopkins LN. Transradial stenting of the cervical internal carotid artery: technical case report. Neurosurgery. 2003;53:448-451; discussion 451-452.
- Bakoyiannis C, Economopoulos KP, Georgopoulos S, et al. Transradial access for carotid artery stenting: a single-center experience. Int Angiol. 2010;29:41-46. Review.
- Mendiz OA, Sampaolesi AH, Londero HF, Fava CM, Lev GA, Valdivieso LR. Initial experience with transradial access for carotid artery stenting. Vasc Endovascular Surg. 2011;45:499-503.
- Mendiz OA, Fava C, Lev G, Caponi G, Valdivieso L. Transradial versus transfemoral carotid artery stenting: a 16-year single-center experience. J Interv Cardiol. 2016;29:588-593. Epub 2016 Sep 16.
- Hopf-Jensen S, Marques L, Preiß M, et al. Initial clinical experience with the micromesh Roadsaver carotid artery stent for the treatment of patients with symptomatic carotid artery disease. J Endovasc Ther. 2015;22:220-225.
- Wissgott C, Schmidt W, Brandt C, et al. Preliminary clinical results and mechanical behavior of a new double-layer carotid stent. J Endovasc Ther. 2015;22:634-639.